Livedo Reticularis & Rheumatoid Arthritis: Nothing Rash about It
Does livedo reticularis have anything to do with Rheumatoid disease?
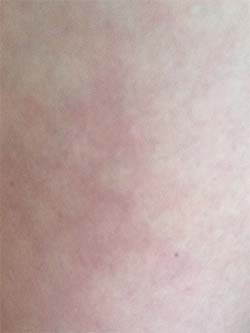 Livedo reticularis is a purplish-colored lace pattern under the skin. There is no raised or itchy rash on the surface of the skin, but the light and dark areas resemble a net-like pattern. The causes and treatments for livedo reticularis are not fully understood, however it is believed that when some small blood vessels are blocked or no longer feed surface tissues, other vessels enlarge to compensate, creating the netted pattern. (See explanations for livedo reticularis on DermNet.)
Livedo reticularis is a purplish-colored lace pattern under the skin. There is no raised or itchy rash on the surface of the skin, but the light and dark areas resemble a net-like pattern. The causes and treatments for livedo reticularis are not fully understood, however it is believed that when some small blood vessels are blocked or no longer feed surface tissues, other vessels enlarge to compensate, creating the netted pattern. (See explanations for livedo reticularis on DermNet.)
Although some sources do not assert any connection to Rheumatoid Arthritis, others do including Wikipedia, listing vasculitis due to Rheumatoid Arthritis and GP Notebook, again listing RA and SLE as possible causes. A Mayo Clinic article lists Lupus as a possible cause, but not Rheumatoid disease. Part of the confusion is this same term is used to refer to a harmless pattern on the skin that is common in cold weather and a more lasting symptom related to vasculitis or other more serious conditions. The condition can also be caused as a side effect of some medications such as amantadine (for Parkinson’s disease) or interferon (for melanoma).
Unidentified vascular “rash” is likely livedo reticularis
For well over a year, I’ve had this vascular rash across the front of my left leg. I asked Dr. GP about it last summer, but it didn’t look very severe that day and I’d already asked a few questions… so nothing was done. Eventually, I asked Dr. Tylenol (a rheumatologist) about it when we went back there last month. Doc looked puzzled, said “Hmm.” I politely insisted it be examined closely, but Dr. Tylenol still shrugged.
I was sure it was vascular because it’s below the surface of the skin. Over the past few years, I’ve had symptoms of vasculitis and my first rheumatologist had noted that in my chart. So I was determined to get some doctor to answer me – even Dr. Google.
Well if you Google “vascular rash” like I finally did and look at Images, you’ll see a thousand rashes, but nothing like my leg. Eventually, I figured out how to describe my leg leaving out the word rash. And I immediately found pictures of livedo reticularis caused by vasculitis related to Rheumatoid disease (or Lupus). Some of them look like my leg, many more severe.
Armed with that information and more pictures of my leg, we saw the GP again last week and doc decided to do a biopsy. The non-rash recently appeared on the other leg as well so I’ll be glad if I have an answer soon – maybe. I asked the GP who treats vasculitis if that’s what this is and the answer was “the rheumatologist.”
Have you had a rash or non-rash like the one in the picture?
What did your doctors say about it?
READ PART 2 HERE:




Your article on livedo reticularis struck a chord with me. I was diagnosed with RA in September 2012. For about two years I had a purplish discoloration on my calf below my left knee. I assumed it was some type of vasculitis, and decided to have ultrasound tests done. The specialist found nothing out of the ordinary for a 62 year old woman, and said the rash was not caused by any vascular issues. My rheumy had no idea what the rash was from, but I was very concerned because over the course of a few months it had spread to my thighs and arms. I then decided a dermatologist visit was in order. Biopsies were taken, and it came back as granuloma annulare. This type of rash (as I understand it) is one in which my immune system is so out of whack that my body is fighting a non-existent condition, and the result is a patchy rash that does not respond to steroid or any other treatment. The dermatologist told me that it is due to my auto-immune disease and could go away tomorrow or not for twenty years. In the meantime, I live in Florida and can’t go anywhere wearing shorts or short sleeves. Something new every day with this disease.
Oh, my. I’ve had RA for mire than 10 years. All of a sudden, about 2 months ago my arms itched so bad I couldn’t keep my hands off them. Some skin patches turned scaly and some changed color. Saw the dermatologist who gave me steroid cream. It helped but hasn’t cured the condition. Right now the tops of both arms itch terribly. No recent change in meds. Embril, plaquinil, gabapentin and Arava. Asthma is a bit worse than usual. Anyone else know anything about this?
At 20 I had a horrible rash from head to toe. It drove me nuts. It was red, itchy and burned. I saw several Dr’s…who didn’t know what it was. The Dermatologist didn’t have any idea either, but decided it had to be an allergic reaction to smoke or that someone had burned poison ivy, oak and/or sumac. Because it itched and burned. He prescribed a concoction of lubriderm and menthol. I had to bathe in epsom salts or oatmeal and then rub the concoction all over. It took forever for it to clear up. No diagnosis of RA at that point.
Move forward about 10 years. While working in the workshop at an ARC, I developed horrible stiff necks that would totally freeze up, to the point that the Dr’s told me when I felt like my head was too heavy for my neck I just had to lay down. That’s totally good for work right? No diagnosis of RA at that point.
Ahead another 5 years. I seemed to be sick all the time. It was like one flu type episode after another. I felt almost every day like I had been hit by a truck! When I would walk my left foot at times would drag and I would almost fall. They finally started testing me for RA…Again no diagnosis of RA at that point either.
Move ahead another 4 years. Went outside in the rain, knee popped and couldn’t walk. PCP sent to an Ortho guy. Dx arthritis, knee injections done…no help. Took a long time to be able to walk unassisted. No diagnosis of RA at that point.
Move ahead another year. While working as an Job Coach, I got to the point I couldn’t walk and I developed a rash above my right ankle. No diagnosis could be made, but this time the PCP sent me to another Ortho guy and a Podiatrist. Re-occuring red flare up on face and cramps under chin.
Dx from PCP possible lupus.
I no longer could stand the pain and told her she HAD to do something.
Dx from Ortho; meniscus tear of my knee…needed surgery
Dx from Podiatrist; broken foot, tendonitis, plantar fascitis and bones eroded in my foot. Referred to Rheumy.
Dx from Rheumy; sero-negative RA, Psoriatic Arthritis, Fibro.
One year later had to get new Rheumy, old one thought that I was exaggerating pain…told if I would lose weight symptoms would clear up. I agreed that I needed (and still do) to lose weight, but that was not the primary cause of my pain.
As I sit here, writing this lengthy comment (sorry) I look at my legs, that have been killing me for the last week, I have a nice purplish web rash on them. Will need to discuss at next Rheumy visit.
hi Claudia, I’m sorry about your rash, but glad to hear you found a better rheum doc!
Oh, my. I’ve had RA for mire than 10 years. All of a sudden, about 2 months ago my arms itched so bad I couldn’t keep my hands off them. Some skin patches turned scaly and some changed color. Saw the dermatologist who gave me steroid cream. It helped but hasn’t cured the condition. Right now the tops of both arms itch terribly. No recent change in meds. Embril, plaquinil, gabapentin and Arava
My rheumy (who doesn’t think I have RA) noticed “livedo” on my legs on my first visit. He said it was no big deal and it happens to some people when they get cold (weird cuz I really wasn’t cold, and my legs are like that almost always). They tend to be worse in the cold though. He mentioned it like three times, each time saying it was nothing to worry about. He also noticed my curvature of my spine. He seemed to be more interested in things that didn’t really matter and it irritated me somewhat. Thanks Kelly for getting the goods once again.
Hi Marti, I love that – “getting the goods” – it’s a mean learning curve, but we figure it out. I’ve read that too about cold, and I think it does happen in a harmless way to many people when they are very cold. I live in Florida and it’s warm usually, but my the livedo ret. is most clear when I’m warm…
In my opinion, what makes symptoms seem more clearly significant is (1) if something represents a change: it was never there before and now it is; so that symptom is not typical with my skin for example. And (2) if something is permanent; I mentioned it to my GP over the months, but neither of us seemed very concerned early on when it would come and go. When it stayed that way permanently.
I have that same non-rash and my doctor also is stumped about it. Thank you! Now I have a name for the “rash” to ask my rheumy about.
I’ve had this “rash” for as long as I can remember, off and on. I remember being told it was not uncommon in fair skinned people, especially in the winter months. I never understood why I would have it when I wasn’t cold. I was diagnosed with RA about 5 years ago. I’ve also had a recurring “rash” that is very itchy mainly on my left arm around the elbow and forearm. Rheum. doc wanted it biopsied by Derm, but it was gone by time I could get appt. I’m on Plaquenil, MTX, and Humira, though off the later two currently due to surgery. I appreciate learning about this. Pieces of the puzzle keep falling into place.
I can comment as both a physician and an RA patient. Livedo reticularis can be seen in a variety of clinical situations from healthy people (often related to cold exposure and more prominent in lightly pigmented individuals) to those with autoimmune or coagulation related disorders. In RA it may reflect a component of vasculitis (inflammation of the blood vessels) but its presence is not necessarily of any clear significance. In general, no additional treatment is necessary beyond appropriate management of the RA. If skin breakdown or ulcers develop, this should definitely be discussed with your rheumatologist. I hope that’s helpful/reassuring.
Thank you very much for your comments.
I don’t know if you’ve read both posts about this, or all the comments I’ve made, but I’ve made exactly the same point also (“no additional treatment is necessary beyond appropriate management of the RA”). In my case, I live in Central Florida which is warm with rare exceptions, and the appearance of the vasculitis on my leg is always worse when I’m very warm (such as after a shower). It is not the same RV that appeared occasionally when I was cold as a child in upstate NY. Above all, it is evidence (as are numerous other symptoms) of untreated rheumatoid disease, as my dermatologist stated.
The point of the other post about this (https://www.rawarrior.com/livedo-reticularis-diagnosis-she-knelt-next-to-me-with-a-medical-textbook/) is that the rheumatologist (and her partner) have no idea what this is, were not curious how the biopsy turned out, and were not the least bit curious when I told them it had appeared suddenly, remained for 18 months (at the time, longer now), or that it disappeared during a 2 month trial of Xeljanz.
Hi everyone, this is my first time here and I’m looking for some answers… My homicidal mother had JRA and spent a lot of time in a wheel chair, she gave me up for adoption when I was a year old so I never got to know her. Anyways, docs say JRA is not hereditary or genetic and they did a lot of testing on me but never found anything.
I’m 28, female, and here’s the long list of things I deal with
– white and purple blotches under skin which very much looks like vasculitis. It comes and goes but seems to get worse when my legs, feet, hands, arms are really hot (sometimes for no reason.) Two of my docs have pointed this out to me but have never said anything more.
-joints hurt (right shoulder- can’t throw a ball, several fingers, sometimes my hip, sometimes my elbow and sometimes my wrist. Currently have a painful bump on top of right wrist and it hurts to put weight on it.)
-Seizure disorder (simple partial seizures, and tonic clonics at night)
-Low blood pressure, fast heart rate, a little bit of elevated cholesterol, and unusually high folate levels in which my GP nor neurologist don’t know what’s causing it.
– Dizziness, vertigo, light headedness but no fainting
-Frequent headaches and migrains
– random cysts and benign tumors in random places on my body throughout my few short years, some have been removed others are still there.
– Goiter on thyroid in which half of it was removed
-Profoundly deaf and wear hearing aids
-Half blind out of right eye, had surgery on it as a baby
-Math learning disorder,
-depression, and ptsd
-fatique and low energy whereas I used to be like the energizer bunny and never stopped moving.
It’s all just simply very bad genetics that I’ve been given but I’m here for a reason and wondering if my docs are just simply not connecting all the dots. There has to be some kind of disease or disorder that has all these things as a symptom. Wondering if my biological mother could have passed on her autoimmune disorder to me??? I wanna know because if it is RA then that means it’s just gonna get worse over time and I’ve got my whole life ahead of me and I should start making realistic goals for my future based on what I’ll be able to handle and not push myself unrealistically to something that will be impossible.
If anyone can help me out here I’ll be forever grateful!,
*BIOLOGICAL mother, not homicidal mother LOL! Crazy autocorrect on my phone!
Hello Kelly, how are you? Sorry for my mistakes in English. .. cause I am uzbek from Tashkent and my English is not good… my name is Bonu… i am 24 years old..I have this problem with my skin about 4 years… livedo…
I walked on many doctors, but anybody long couldn’t make the diagnosis. . all analyses were in norm… to me prescribed medicine which strengthens vessels and all… spots increase… any more only on a shin, but also on hips. . help me… how to stop it? it will be on all body?
I don’t think it will spread to the whole body, but please talk to your doctors – Especially if the medicine made it worse.
Hi, I can accross your site, doing the same as you were, desperately trying to find an answer for my “spotty legs” I’ve been like this since a child, and very embarrassed going thought high-school. Always wearing pants or thick stockings. My doctor brushes it off all the time, and I’ve asked her 3 times to address it. She say’s it’s nothing at all to worry about. I also have terrible digestive issue and i wonder if I have auto-immune issues too. I would just like to improve it, it seems to get worse with age… Any updates/news?
I have had this “rash” for about 12 years. It started with a PE when I was 30. From there I have fibromylgia and my feet and fingers, lips go blue! I have had a rash on my face since I had surgery 4 months ago. My GP says nothing
I don’t know what to do any more
I’m just in pain all the time
I’m sorry you’re in pain all the time Noreen. It does get old.
Have you asked another dr about the blue fingertips? That is a symptom of Reynauld’s syndrome, which is not uncommon w/ rheumatoid. If the GP or the rheum doc doesn’t know, you could ask a dermatologist. The rash could be some kind of inflammation triggered by the surgery, but you should have it checked out by someone who knows how to identify it since rash on the face is a symptom of lupus.
Hi Kelly,
I have had this on my lower legs. Mine usually appears each summer. My Rheumatologist looked at it and said that it is vaculitis from my sjogrens. He was not concerned at all about it. Apparently there are multiple causes for this.