It All Comes Out in the Wash: Comparing Different Treatments & Approaches
 Four weeks. Not a record for me, but close… When this is published in the morning, I’ll be spending the morning washing and blowing out my hair for the 1st time in about a month.
Four weeks. Not a record for me, but close… When this is published in the morning, I’ll be spending the morning washing and blowing out my hair for the 1st time in about a month.
The ends started to take dreadlock form the last few days, somewhat an improvement. But the front looks really bad [deliberately not in photo]. My neck is a bit better today and I’m going for it! It will be a very long day of errands, meetings, and phone conferences, but it will feel good to look “normal.”
Does that sound random? Bear with me.
Yesterday, I was speaking with someone who needed to understand RA patients’ point of view for her project for a pharma company. And she didn’t (understand).
Giving her free advice, I told her that my neck and hands have hurt too much to make it worthwhile to wash my hair. She hesitated to believe me, maybe because she’s been told that medication helps everyone with Rheumatoid disease to feel close to normal on most days, with maybe occasional flares.
Finally, I told her: Look, there is a small percentage of people who have remission or mild RA who can do the things you suggest, but that is not your audience anyway since your drug is for people with “moderate to severe RA,” right? Make sure you don’t insult anyone…
Of course, people with RA do not yet have THE silver bullet. And researchers know that. That’s why they investigate how treatments stack up against each other. Here are two interesting studies I’ve read recently.
Seeing “very little difference among the current biologics”
In “Abatacept versus other biologics in methotrexate inadequate responders with rheumatoid arthritis: you like tomato and I like tomahto… let’s call the whole thing off,” Yusuf Yazici (a colleague of Dr. Ted Pincus), comments on current studies that compare biologics: “(A)s far as efficacy is concerned, there is very little difference among the current biologics.” Yazici says there are more pressing matters to explore to improve patients’ lives. “It is time to stop picking favorites among the biologic agents and focus on how we can get more physicians to monitor RA outcomes that would allow us to be as aggressive as RA demands us to be.”
Comparing less expensive triple DMARD therapy to Enbrel plus methotrexate
Over several years, the TEAR Trial has examined early, aggressive RA to compare oral DMARD combination therapy (methotrexate, sulfasalazine, and hydroxychloroquine /Plaquenil) to methotrexate plus etanercept (Enbrel), asking:
- Whether any combination therapy (three DMARDs or methotrexate with etanercept) is more effective than methotrexate alone, with a step-up approach.
- How does combination therapy compare to methotrexate plus a TNF Biologic?
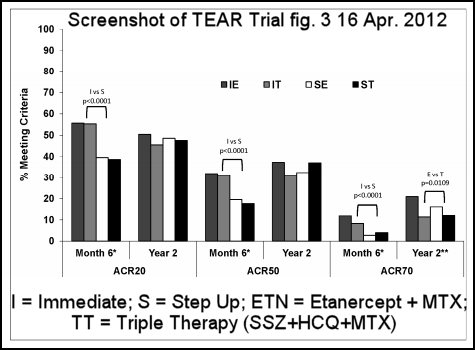
“The treatment of rheumatoid arthritis (RA) has changed dramatically over the past decade” and there is a need to know whether one approach is proven to be more effective, especially considering how costly Biologics are. The primary outcome of the trial was the popular disease activity score, DAS28-ESR between weeks 48 and 102, and this showed no difference between the two treatment approaches. However, the etanercept plus methotrexate patients had a “smaller increase in radiographic scores” (x-rays of hands, wrists, and feet).
More interesting points: “We observed a higher rate of participants not completing the study than we had originally expected.” Dropout rate was 32.1%, and most of those who decided not to continue cited lack of efficacy or did not provide a reason. The screenshot of figure 3 shows that both immediate therapy (IT or IE) groups had more patients who reached ACR response levels than those with step-up approach.
Nope. No silver bullet yet. Of course the marketing folks can’t talk to the researchers, but I wonder whether the researchers laugh when they watch the commercials that make treatments seem like a cure. Anyway, I hope both of them will talk to patients more.




My pain in my neck, hands, wrists, elbows& shoulders has been so bad I’ve been thinking about braids or a weave do I won’t have to wash my hair every few days. I went natural for easier maintenance and to showcase my natural curls, but it takes upkeep too. No curling irons but detangling…I’ve been close to locs too. But I haven’t decided to locus hair yet! Lol! Thanks
Kelly for always sharing and educating. (((hugs))) sister!
I grew my hair out specifically so I could pull it back into a ponytail and look put together. I didn’t have the energy for doing anything to it even every other day. Now it is so long I’m running into a new problem: it would work better in a braid, or even better a french braid, but I’ve discovered I now longer have the ability to work my hands behind my head to do it. I may have to teach my husband how to do a french braid and have him do it for me some days before work.
Anyway, ARGH on the not getting it. I think that drug rep just doesn’t understand just how serious autoimmune diseases can be. It’s not like a headache. Sheesh.
Kelly, I understand. Some days I don’t even feel up to getting dressed, and I stay in my comfy PJs till the body starts to loosen up…
Re the studies: what always strikes me are the ACR 20/50/70 criteria (20%, 50% or 70% improvement.) There are so relatively few who get to 70%, and even that is not remission.
I was very lucky to be at probably 70% improvement on Enbrel but unfortunately had to go off it because of adverse effects. But 20% as a criteria? My symptoms vary hour to hour, day to day, and I am sure there is a 20% variation even without change in meds, so it seems a very weak criterion. Although I understand that for some it may mean the difference between getting through the day vs. being immobile, but still… to consider 20% improvement as a satisfactory response seems an over-reach, and contributes to the misconceptions about effectiveness of treatments.
All good points and arguments I’ve included in discussion as I present our point of view. And all of these terms are relative and subjective, even joint counts are not objective measures becuase patients “count” differently than drs count. Another confounding factor: some people have only some joints affected. Others have all joints affected. So, the measures do not directly compare.
I don’t know how people would react, but I don’t really have “good” days physically so I work in pj’s or sweats pretty much all the time at home. Getting dressed is one of the hardest parts about traveling because once I’m dressed I want to go lie down, but the day is just beginning.
I fully agree with how hard/tiring and painful hair washing and drying is.I find that sometimes hair washing etc. is my main goal/achivement of a day. The worse the R.A.D has got the shorter my hair is!
I’ve not washed my own hair in years, my fiance does it for me. I cut my hair short a few years back as I was struggling to look after it, but I do miss slightly longer hair.
I’ve just been reading http://www.dana.org/news/cerebrum/detail.aspx?id=36272 about a new non-chemical treatment. Check it out! It certainly gives me hope.
It’s not pretty, but it’s the truth…. it should be in an RD commercial…
I’m having a bad fibro fog day today, so forgive me if I’ve posted this before, but thank you for addressing not only the med situation, but also the fact that the pharma companies seem to have no idea what real people with auto-immune diseases deal with. I hate those stupid Enbrel commercials with Phil Mickelson, because my sons will see them and ask why I don’t take that so I will be better. It is such a dis-service to those of us who are crippled and suffer daily. It’s difficult enough to explain RA to all of those who confuse it with regular arthritis, without the drug companies proclaiming that if you only took their brand you would be perfectly well again. Thank you for representing us so beautifully. God bless. Gay Nell
Short hair here too. Too many other things to try to do in a day. I prefer no worry about hair, or shoe laces. Just getting socks on is enough on the bad days.
You are so right about the hair. I’ve had what I like to refer to as my “dreadlocks” many times over the years. Medium length,curly,humidity…Yep, they were right there on the neck. But I have learned to love them. Who wants to look “polished” anyway? Glad you could do your hair again.
I was part of the TEAR study out of University of Alabama, Birmingham. I took active part in the study for 2 years. Had just been diagnosed with Agressive early RA, thank G-d for my wonderful clinic who takes part in studys. The pain, fatigue and being very frightened went away very quickly. I don’t know which drugs plus Mtx I was on the first 18 months, I only know that in the last 6 months of the TEAR study I took Enbrel and methotrexate once a week. I had to mix my own vials and learned how to inject. My Dr. said they were seeing if heavier doses with biologic drugs + Mtx in the very beginning was more effective than increasing the drugs as the disease progressed. In my case it was more effective. It knocked my inflammation and joint damage down and carried the results over 3-4 years while taking 8 tabs of Methotrexate only, once a week. I’ve been back on Enbrel again for 1 1/2 years and doing well. Blood work done every two months is fine. My sed rates continue to go up and down, but we don’t know why. My Dr. said we will rely on my description of how I feel and how active I can be. When I asked about my general progression and what I might expect in 5 years from now…..my Dr. replied, “I am very optimistic”. (words I love to hear)
All that “vanity shall come at a price…” not only did I never believe it – I thought it was ridiculous.
Until vanity did indeed have a painful price- urhg… I know I hate a whiner too – but it’s just plain unfair that a girl has to blow dry with hands that have recently been run over by several trucks. Agreed?
it’s worth it – fresh hair – high heels- blessed be- but hell on the getting.
Breanna
Thank you….this is all I can manage to say. Thank you, Thank you, Thank you. For the past 5 years I have been beating myself up mentally and blaming myself and my being weak on various mental aspects of myself….I’m lazy, I’m dumb, whatever the day brings. You have made me realize it’s not me….it never was, and I am not the only one going through this.
After 31 years of suffering with RA, the past 5 being the worst…you have given me relief in knowing I am not a bad person or a weak person. I am a fighter, and I’m not the only one getting beat up every day because of it. Thank you
Thanks for your very accurate and humorous take on RA. Sad that they seem to get it wrong all over the world. I’m in South Africa and also going through the 40 pills a day regime. I told my Specialist my tablets caused me to vomit non-stop for 3 weeks(lost 20 pounds). She looked at my wrists and said:” AT least it’s working – you’re joints aren’t as swollen anymore!”…Yes…I am SOOO happy the treatment is working so well 🙂
So true!!! Now I can hold myself up over the toilet as i puke. That IS so much better. Hope the 40 pills a day work. Keep in touch.
Kelly
I am so thankful for your wonderful site. It helps me get through many days when I realize I am not alone. The info is so helpful and I love the humor in so many posts. Gentle hugs to all!
We started my therapy after about two months of testing and observation when it was decided on inflammatory arthritis later RA. Beginning with methotrexate oral going up to 25mg given along with folic acid and then leucovorin for the nausea. A bit later we moved to sub q injections. I had no problem injecting because I was a nurse in my past life, I was given multi dose vials that I used up. A year later we started Humira every other week. Changes happened as the methotrexate caused liver issues and by the fifth year methotrexate was withdrawn and replaced with Arava and that has gone up in dose and back down with liver issues. By year 11 I wasn’t getting the same results from the Humira and Arava. New testing took place and I have moved to Orencia infusion and Arava three days in a week.
Generally I am feeling better but the one thing that hasn’t gotten better and often gets worse is the fatigue and energy. Pain comes and goes and varies with what I do or don’t do. Movement is key for me. Working with my hands above my head like working on my hair saps my energy quickly as well as shoulder and neck pain. Glad I have short hair. Until recently it was short enough that I could just wash it put in gel and fluff with my finger, usually no drying. But now my hair is a little longer in a wedge because I got tired of seeing my scalp from the thinning from drugs. Now it doesn’t look nice unless I blow it dry. I sit and blow for a while before going to mirror to finish.
Everyone with this disease needs to learn new ways to do things, it’s an alteration from our past lives. But it can be done once you find out what works best for you and then sometimes you have to get real and give up some things. That’s ok too.