Sternoclavicular Joint Involvement in Rheumatoid Arthritis: Fascinating Discovery of a “Neglected Joint”
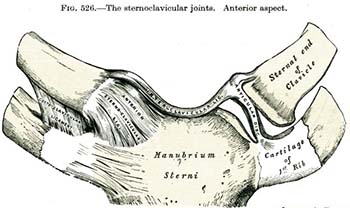
About a month ago, I was fascinated by a new report on 103 “patients with Rheumatoid Arthritis” in Mexico, “Sternoclavicular Joint Involvement in Rheumatoid Arthritis: Clinical and Ultrasound Findings of a Neglected Joint.” A sternoclavicular (SC) joint is a joint at the top of the sternum that allows movement of the clavicle. We each have 2. You can view clear pictures of the SC joint on Shoulderdoc.co.uk.
How often are sternoclavicular joints affected in Rheumatoid Arthritis?
 This is the first modern study on the prevalence of SC joint involvement, evaluating joints in several ways:
This is the first modern study on the prevalence of SC joint involvement, evaluating joints in several ways:
- Visual inspection
- Palpation (touching) during rest and movement
- Asking about history of pain or swelling
- Listening for crepitus (which can be done with a stethoscope as seen here)
If they found any of these, researchers considered the SC joint to be “clinically involved.” Their exams detected that 19% of SC joints were clinically involved, compared to only 1.9% in a healthy control group. The SC joints were also thoroughly evaluated by specialists with musculoskeletal ultrasound (MSUS). 43% of SC joints had at least one MSUS lesion, compared with 17% in the control group.
They concluded that “The sternoclavicular joint actively participates in the systemic inflammatory process of rheumatoid arthritis, as do other peripheral synovial joints,” and that ultrasound is an effective tool to identify it.
Ok, that’s interesting to know about, but why does it matter?
Why this story is valuable to patients
- The study authors acknowledge a model of a “clinically affected” or “involved” joint. It would be a significant improvement in care if this model were widely used. I’ve advocated consideration of involved joints (including any sign of involvement) because it would provide a more accurate picture of a particular patient’s disease. It is more precise than merely counting which joints appear swollen in a clinician’s opinion at a particular moment.
- Crepitus is acknowledged as a meaningful symptom. I’ve heard and read from some rheumatologists that it is not to be considered significant.
- Expert musculoskeletal ultrasound was used to detect signs of disease activity that are not always obvious. (More on that soon.) Diagnostic MSUS is very valuable if performed by a well-trained clinician, as RAW has reported, and not yet widely available in the United States.
 How can there be a “neglected joint” in the first place? Why do people who live with a disease know things that experts who write textbooks don’t? After listening to experts for the past few years, I have some ideas (listed below). But first, a telling little story:
How can there be a “neglected joint” in the first place? Why do people who live with a disease know things that experts who write textbooks don’t? After listening to experts for the past few years, I have some ideas (listed below). But first, a telling little story:
Last year, I shook hands with one of the top rheumatology experts in the world using my usual safe handshake that doesn’t allow fingers to be squeezed. Then he pleasantly explained to me that his RA handshake version was better since “RA doesn’t affect DIP joints,” and he proceeded to firmly squeeze the end half my sore fingers. With a smile, he thought he taught me something new because it never occurred to him that some people (actually most) do have DIP joints involved.
What ELSE can be learned from this study?
Look at this simple sentence: “Both the patients and healthy controls were specifically asked about the current or past presence of signs or symptoms reminiscent of SC joint involvement (i.e., pain and/or swelling).”
- More is unknown than is known about Rheumatoid Disease, as many freely admit. Therefore, it is irresponsible to tell patients “such-and-such joint is not related to RA” or “that symptom cannot be your RA,” etc. as patients often report. See also DIP joint.
- The most valuable input to assessing Rheumatoid Disease is the input of the patient who lives with it 24/7/365.
- The most important quality in a researcher is intellectual curiosity, so that she or he is open-minded to things that are not already known. Intellectual curiosity enables researchers to ask new questions or examine them in new ways, instead of protecting the existing framework. Without honest curiosity, advancement of knowledge is very slow. Intellectual curiosity is the polar opposite of dismissiveness too often seen with RD.
Recommended reading
- Does It Matter Whether Rheumatoid Arthritis Affects DIP Joints?
- What Is the List of Rheumatoid Arthritis Joints?
- Posts on musculoskeletal ultrasound (MSUS)
- Rheumatoid Arthritis Hand – Safe Handshake
Pedro Rodríguez-Henríquez P, Solano C, Peña A, León-Hernández S, Hernández-Díaz C, Gutiérrez M, Pineda C. sternoclavicular joint involvement in rheumatoid arthritis: Clinical and ultrasound findings of a neglected joint. Arthritis Care Res. 2013 Jul [cited 2013 Jul 30];65(7):1177–1182. Available from: http://onlinelibrary.wiley.com/doi/10.1002/acr.21958/full. Abstract available from: http://onlinelibrary.wiley.com/doi/10.1002/acr.21958/abstract.
Yood RA, Goldenberg DL. Sternoclavicular joint arthritis. Arthritis & Rheum. 1980 Jan [cited 2013 Jul 30];23(2):232–239. Available from: http://onlinelibrary.wiley.com/doi/10.1002/art.1780230215/abstract




I feel that this is a great step forward for us because it gives us something we are forever seeking as patients: validation. It would be wonderful to see the use of Ultasound become a standard in Rheumatology offices because so many of us have pain that is truly invisible. I wish we could be there to see the reaction of certain experts as they discover that RA does, in fact, affect the DIP Joints, the Spine, and other joints which we have been often “reminded” are not affected.
I’ll write about ultrasound again soon, but yes you are so right Dori – It’s a shame how people with this disease are often dismissed because there is not yet “obvious” damage & when US would prove the disease activity.
Some forty or so years ago, back when my arthritis was “merely” rheumatic and palindromic, I suddenly developed sharp pain in my sternum. The pain didn’t “do” any of the things that heart-generated pain was supposed to do, e.g., radiate down an arm, so telling my self that heart trouble was impossible for a woman in her twenties, I ignored it. When it spread to my ribs on both sides, I knew that it was my old adversary, RA, that this winter had chosen a home in my sternum and ribs rather than my feet, and avoided the futility of seeking medical help at that time for a pain that “couldn’t possibly” be located there.
yes, and I wouldn’t be surprised if you have inflammation in the joints between your ribs and the sternum too.
I, too, have come to terms with costochondritis and that it does live there, along with many other places not readily recognized by most rheumatologists. After being diagnosed with JRA in 1985 ,at age five, and living with this disease for thirty-five years now, it’s sad to see how much knowledge is being lost from our physician’s of yester years that knew this disease’s potential up close and personal back when it didn’t have the treatments available today that do such a good job at preventing newer cases from advancing stages so radically more often. Most doctor’s that I’ve come across today can’t even comprehend how treatment was for us before biologics, yet alone methotrexate. Though it’s unfortunate that patient’s had to suffer to the extent that they did, before these miracle drugs were options (and, of course, for some they still aren’t options) doctors saw more to the extent of how this disease ravages the body when it’s not controlled and they utilised tools that I just don’t see being implemented today that are still relevant to this day and have a place for patients if more doctors were aware of them. Drugs alone didn’t keep me out of a wheelchair by the time I was sixteen. Drugs, rehab, therapy, surgery, resting splints, and the educational resources that was implemented with all of those did. It was carefully planned and executed coordination between all my healthcare professionals, my support system, and myself that I have to thank for getting me through the first half of my life with JRA. The second half is a much different story.
I was recently sitting in my rheumatologists’ waiting room reading the article, “Biologics: The Turning Point” by Mary Anne Dunkin from ‘Arthritis Today’, the May-June 2019 edition, when I was taken back by a quote in the article from Karen Onel, MD, chief of pediatric rheumatology at the hospital for Special Surgery in New York City. The article says that Dr. Onel is glad the pre-biologics era is in the past. She states, “I am the last generation that will remember what it was like before biologics. We used to spend half our time teaching fellows about rehab and braces. The truth is we don’t do that stuff anymore – our patients just get better.” My question to doctors and others who think in such matter of fact terms is what about the patients who don’t just get better? What about the patients who can’t take a biologic for whatever reason? What about the patients who will need those braces or that rehab? Will your fellows, future doctors, be able to recognize when to utilise these tools if you “don’t do that stuff anymore?” Those tools work. They are tried and true and are a testament to patients abound. Before they are discarded as outdated, perhaps healthcare professionals shouldn’t assume all their patients will hold fast to one type of treatment. In my opinion, specialists can stand to have all tools available in their for their patients when treating any illness, but especially crippling ones.
I was so happy to read your post about the SC joint.
I have had swelling there and pain. My x ray did not show much even though the swelling was visible with the naked eye.
My doc did say he thought it was the RA. I also have been dealing with cervical spine problems.
I really feel that RA has affected many joints that are not identified as RA.
I had a nuclear bone scan that the radiologist read and showed the dye or lite up areas were:
bilateral wrists, knees, ankles, fingers, toes, and also the shoulders.
But, he said it was from my osteoarthritis???????
I called the hospital to let the technician that gave the films to the radiologist that I have RA, not just OA.
Only then did they add an addendum about it being RA.
Still, it amazes me that professionals do not know what is RA and what is not.
Hi
I am new to the RA scene and have been doing heaps of research on medications t take. I am lucky and have 9 months to decide on a course of action. I did come across this natural supplement and was wondering if anyone had heard of it. The name is cerasomal-cis-9-cetylmyristoleate (CMO).
I am sorry if I posted this in the wrong area but could not find another place to post. Any help would be much appreciated.
Thanks
hi Ashlea, I’m not sure what you meant about having 9 months to wait. I hadn’t heard of the CMO so I looked it up. It looks like that supplement has been around a long time since I saw the U.S. Federal Trade Commission registered a complaint back in 1999 for false claims http://www.ftc.gov/os/1999/09/arthritiscmp.htm. As far as I know, if it really is rheumatoid disease that you are developing, there is not any supplement that can treat it. Of course there are important things we can all do for our health, but I wouldn’t see it as the same thing as disease treatment.
Hi Kelly,
Thanks by 9 months I mean I am just in early pregnancy and cannot take anything. So far my symptoms have become a pain level of three instead of ten! CMO- well I don’t know, I am thinking of taking sulfasalzine. Have you had that before?
No I haven’t taken that because I’m allergic to sulfa drugs. Best of luck with the baby!!
hello kelly,
wow i have had “muscle strain” when young, “fatigue” when a little older, a trip to ER in my 40’s and fighting fear because i know it can’t be heart attack several times since.
this is curious and unfortunay logical. next time i get that strange pain i will know for sure it is RA and not have to fight fear in addition to other emotion.
again thankyou
Kelly, this news about the shoulder being affected by RA is particularly interesting to me, because I have recently been diagnosed by an orthopedic surgeon and a d.o. As having an irreparable torn rotator cuff in my right shoulder. Four tendons are torn and the MRI shows that three are old tears. I have been doing pt and exercises in my pool but nothing helps either the pain or the functionality. The doctors feel that for quality of life I ought to think about a shoulder replacement. Having had a knee replacement in 99 and a titanium rod inserted in my spine in 2009, and am much improved from both, I’m not opposed to surgery. I haven’t even discussed this w/my rheumy or my primary physician as I didn’t think it had anything to do w/RA. But I’ve had shoulder pain for decades and was diagnosed w/RA in 97. I am now 74’and this damn disease wallops me daily, but I’m not ready to give up yet. I have stories to write about and a life to live!
Incredible! It never occurred to me that rheumatologists were not aware that RA can affect every joint. I’ve had inflammatory involvement of all my ribs and my sternoclavicular joint since onset. By now, nothing should surprise me. But it does.
Kelly I’ve been searching for anyone who has trouble with their nose. Can’t find anything. My nose gets full of scabs and when I take a shower they soften up and come out . Gross I know.. My nose is so raw and itchy! I’ve been putting antibiotic cream in it but its not working. Have you heard of this from anyone or yourself? It’s becoming a real problem with me! It hurts! Thanks Kelly
are you taking methotrexate? if so how much folic acid do you take? I have heard of nose sores from that. Did you ask a dr yet?
Also one thing that might help it heal up is a little zinc oxide applied with a q-tip very gently. I might do the antibiotic at night and the q-tip after showers.
Is this site / blog still active?
indeed