The Cricoarytenoid Joint and Rheumatoid Disease
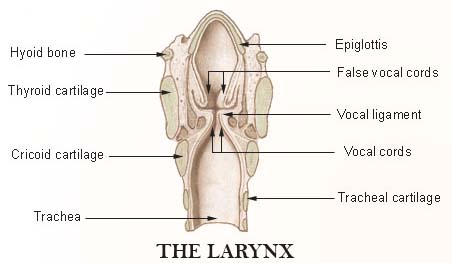
Speechless… the cricoarytenoid joint is commonly affected in Rheumatoid Disease
Recently a small study from Brazil raised the topic of cricoarytenoid arthritis (CA), a little-recognized aspect of Rheumatoid Disease. In 2009, RAW first discussed CA with patients who expressed amazement that their vocal cord / larynx problems were related to their Rheumatoid Disease. There are a couple of hundred comments on CA on RAW, although I seldom mention it.
Cricoarytenoid arthritis is a broad term referring to several ways that Rheumatoid Arthritis / Disease can affect the larynx, or cricoarytenoid joints. See list of cricoarytenoid symptoms below. Unfortunately, CA has frequently been supposed to be rare or inconsequential, and symptoms are often dismissed.
“He looked at me like I was an idiot and said ‘But there are no joints in the voice box.’”[1]
The role of cricoarytenoid arthritis in Rheumatoid Disease
 The Brazilian study sought to investigate the inadequacy and inconsistency of research on how Rheumatoid Disease (RD) affects the cricoarytenoid joints.[2] I’m always grateful for doctors like this who show curiosity to learn how RD actually affects people. Let’s have a look.
The Brazilian study sought to investigate the inadequacy and inconsistency of research on how Rheumatoid Disease (RD) affects the cricoarytenoid joints.[2] I’m always grateful for doctors like this who show curiosity to learn how RD actually affects people. Let’s have a look.
They said –
- “Rheumatoid arthritis (RA) is a chronic, autoimmune disease, of unknown cause, which affects mainly women between 30 and 50 years of age.”
- “Knowledge on the laryngeal involvement in RA patients is longstanding: the changes were described by Mackenzie, in 1880, by means of studies in cadavers…”
They found –
- 80.9% of Rheumatoid patients reported at least one CA symptom
- The prevalence of dysphonia and videolaryngoscopy changes was respectively 12.8% and 72.4% in patients with RA.
- Posterior laryngitis was the most common diagnosis (44.7%)
- Patients with a higher DAS score did not have significantly more laryngeal involvement, so…
They concluded –
- “This study showed that laryngeal symptoms and laryngeal alterations are frequent in RA patients”
- CA can compromise an individual’s quality of life
- Dysphonia in RA individuals is more prevalent than in the general population (less than 1%), and less prevalent than in those with laryngeal diseases
- “There was no significant relationship between laryngeal disorders and disease activity” (i.e. arthritis symptoms as measured with DAS)
Don’t miss 2 significant details
1) “No relationship between laryngeal disorders and disease activity” is unfortunate wording that results from measuring a systemic disease by counting swollen fingers. The critical point here is that extra-articular disease (CA) is not shown to correlate with joint disease activity (arthritis). This underscores the importance of improving measures of disease activity in order to capture a more complete picture of the health of patients.
2) “Could medications be to blame?” the investigators wonder. It is doubtful since many people experience CA before they are ever treated for RD. Furthermore, CA was documented long before modern treatments existed.
Possible symptoms of cricoarytenoid arthritis
- Hoarseness / laryngitis
- Painful swallowing (odynophagia)
- Feeling of a foreign object / lump in the throat (globus pharyngeus)
- Sore throat
- Cough
- Difficulty breathing (dyspnea)
- Change in sound or tone of voice (dysphonia)
- Loss of voice (aphonia)
- Pain during speaking
- Pain during swallowing (dysphagia)
- Choking sensation
- Stridor (high pitched sound caused by difficulty breathing)
Concerns of cricoarytenoid arthritis in PRD
- Voice changes or difficulty singing may affect employment.
- CA can be painful or uncomfortable; “Both dysphonia and RA may compromise an individual’s quality of life.”[2]
- Sometimes CA requires injections or surgical intervention such as tracheostomy[2]; PRD in our community have given testimony of both.
- Anesthesia complications: CA may make intubation difficult or lead to postoperative exacerbation.[3]
- Rarely, CA can be life threatening. Patients need to be honest about symptoms with doctors they can trust.
Recommended reading
- What Is Crepitus in Rheumatoid Arthritis / Disease?
- Does Rheumatoid Arthritis Affect Tendons?
- Rheumatoid Symptoms Persist Despite Treatment: a Study in Juveniles (JRA / JIA)
- Forefeet and the DAS28: a Healthy Dose of Skepticism
MORE
- Cricoarytenoid Arthritis in Rheumatoid Arthritis, Part 1
- Cricoarytenoid Arthritis in Rheumatoid Arthritis, Part 2
- Cricoarytenoid Arthritis in Rheumatoid Arthritis, Part 3
FOOTNOTES
1 Patient comment. 2013 Apr 17 [cited 2014 Jan 28]. Available from: https://www.rawarrior.com/cricoarytenoid-arthritis-in-rheumatoid-arthritis-part-1/?show=comments#comment-203637
2 BeirithI SC, ; IkinoII CMY, Pereira IA. Laryngeal involvement in rheumatoid arthritis. Braz J Otorhinolaryngol [Internet]. 2013 Mar/Apr Laryngeal Manifestations of Rheumatoid ArthritisLaryngeal Manifestations of Rheumatoid ArthritisLaryngeal Manifestations of Rheumatoid ArthritisLaryngeal Manifestations of Rheumatoid Arthritis[cited 2014 Jan 28];79(2). Available from: http://dx.doi.org/10.5935/18088694.20130040
3 Fombon FN, Thompson JP. Anaesthesia for the adult patient with rheumatoid arthritis. Contin Educ Anaesth Crit Care Pain [Internet]. 2006 [cited 2014 Jan 28];6(6):235-239. Available from: http://ceaccp.oxfordjournals.org/content/6/6/235.full




This is so interesting. At about the time my symptoms were getting worse ( pre diagnosis ) I found I couldn’t sing along with my favorite songs on the radio anymore.
Thanks for posting, interesting read. Prior to my official DX and when I was only 16 years old I developed a “stone” in my throat, after seeing several Dr’s, my parents had found the right one, by this time, almost a year had passed. The “stone” would swell whenever I ate, so I didn’t eat much! When I did, I resembled a bullfrog. The Dr. That removed it tried to go in under my tongue, but was unsuccessful, he ended up removing the stone and the entire glad from my neck. The stone was the size of a golf ball by the time they removed it! At any rate, everyone with RA should be aware that throat problems should be checked if there is any concern.
I’m with Bonnie – about the time of diagnosis I could no longer sing and at times my voice is very hoarse. Have asked two rheums about it and was told by both ‘it’s not related.’ This is the first place I’ve seem people talk about it.
Very sad to hear of rheum docs who do not know about something so common. It does not get into the medical records, and then it continues to be called “rare.” An ridiculous vicious cycle. I remember the first couple of years singing silently (lip synching) only. Now my voice comes & goes.
I was diagnosed at age 56 last May. My symptoms began in mid-April with swollen and painful fingers (even distal joints), thumbs, wrists, neck, and knees. I also noticed that my voice was different. I’m a lawyer and talk for a living, but I also sing in a semi-professional church choir. In mid-April, with all of those other symptoms, my voice changed. I could not sing in my lower range without forcing it and it didn’t sound normal. Once my GP prescribed prednisone and I saw a rheumatologist, my voice returned to normal. I told the rheumatologist about my voice, but she appeared to dismiss it like the pain in my distal finger joints.
It explains why lately my voice is different. I have a sore throat on and off for the last couple of days without any obvious infection.Just this morning I was talking to a friend on the phone and I noticed my voice was unable to reach lower registers and it hurts a little when I try to force it. I use to sing as well. I won’t even attempt it and haven’t in years. So what to do about it then?
Jennifer, ideally whatever disease treatment works for your other symptoms would improve any vocal cord symptoms as well. If a person with RD has CA, it would be a sign that the RD is not “controlled.”
If the symptoms are extreme, sometimes doctors inject steroids into the larynx.
I am so grateful to you for shining a light on this topic. Years ago, I used to get laryngitis all the time and sometimes unrelated to having a cold. It got better after I found a treatment that works for my RA, but my voice still gets strained easily. It’s also become the first sign of my asthma becoming triggered by e.g., paint fumes. Instant loss of voice, which never happened before the laryngitis.
I am a speech-language pathologist by training with 30 + years of professional experience. I have rheumatoid disease. Speech pathologists have a fairly good working knowledge of the anatomy and physiology of the throat. I knew there was some disease process happening in my throat. My throat symptoms began with difficulty swallowing-but not all the time, extreme pain along the left side of my throat, and a lump-like feeling in the throat.
Like others, my symptoms were dismissed. Many rheumatologists are not that skilled at matters of RA and the throat, it seems.
I was seeing a sinus specialist for chronic sinus infections. He recommended I see an ENT (Ear Nose Throat) doctor – also called an Otolaryngologist. A CT scan of my throat was ordered (the standard imaging test for RA and the throat). The ENT looked at the actual CT scan and said my cricoarytenoid and cricothryroid joints were not involved. He examined my vocal cords (another area of involvement from RA). He said I did not have vocal nodules or any pathology from RA in the vocal cords. He saw redness in my throat and some inflammation. He asked me a lot of questions and also used a scope to look down my throat and film what he was seeing.
The ENT gave a working diagnosis of gastro-esophageal reflux disease (GERD). I was given a one month trial course of Tecta medication. I came back to the ENT for a follow-up appointment. He did another scope of my throat and asked me how I was. The tecta had only a modest effect on my symptoms. The ENT wrote in his report that “the oral cavity, pharyn and larynx are structurally normal” BUT….. “rheumatoid disease is affecting her esophageal motility”. This means the joints of my throat and my vocal cords are normal BUT….. RA is having an impact on how my esophagus works.
So, the important thing here is that RA is not just a joint disease, as we know. When speaking about the throat, RA DOESN’T ONLY AFFECT THE CRICOTHYROID OR CRICOARYTENOID JOINTS in the throat. RA can actually affect how the throat itself functions – how the different parts of the throat move, how the vocal folds come together, how food moves down the esophagus.
Throat symptoms can be due to many other disease processes other than or in combination with RA. It is VERY important to believe in yourself and what you are experiencing if you have throat symptoms. PLEASE ask for a referral to an ENT who specializes with the throat (some specialize with ears, some specialize with sinuses, etc….). If you can’t find an ENT, see if there is a speech-language pathologist in your area who specializes with voice problems. They work closely with medical specialists and can likely help get you the proper medical treatment.
Here’s a list of research references on RA and the throat for those wanting more information.
Laryngeal Manifestations in Rheumatoid Arthritis
References 2013
1. Stojanavic and Belic (2013) http://cdn.intechopen.com/pdfs/41621/InTech-Laryngeal_manifestations_of_rheumatoid_arthritis.pdf
RA in the larynx can manifest in the following forms: Quote from Stojanavac, page 228-229
a) Arthritis of cricothyroid and/or cricoarytenoid joint (Ferdynus-Chromy, 1977; Gotze,1973; Kubiak-Socha, 1973; Woldorf, 1971; De Gandt, 1969; Copeman, 1968),
b) Rheumatoid nodules (Bridger, 1980; Bonner, 1977; Abadir, 1974),
c) Laryngeal myositis
d) Neuropathy of laryngeal nervus recurrens and
e) Postcricoid granulomas (Bienenstock H, 1963).
Histological examinations of cricoarytenoid joints in RA have shown synovitis as the earliest change that leads to synovial proliferation, fibrinous deposit, forming of pannus on joint surfaces, erosion of the joint cartilage and finally obliteration and ankylosis of joints.
Cricoid necrosis as the last phase of pathological changes on the cricoid cartilage can cause serious pathophysiological disturbances (Gatland, 1988).
Neural atrophy of laryngeal muscles and degenerative changes in laryngeal nerves caused by vasculitis, can follow the degree of affection of cricoarytenoid joint (Voulgari PV, 2005; Lofgren RH, 1962). Rheumatoid nodules of different size in the larynx-are mainly found with seropositive RA.
2. Lene Anderson , great article. Also see references at the end of the article http://www.healthcentral.com/rheumatoidarthritis/c/72218/161985/hoarsenessra
3. Chen 2005: http://www.ajnr.org/content/26/4/970.full.pdf
4. Gates 2006 http://radiographics.rsna.org/content/26/1/e22.full
5. Hamden 2007 http://www.meja.aub.edu.lb/downloads/19_2/335.pdf
Sally, thank you for all of the information! Do you happen to know how RA of the larynx is distinguished from symptoms of Wegener’s? I have had the issues with my voice and throat (and breathing difficulties/ intermittent choking) forever it seems. I’m now in the midst of testing with different specialists disagreeing in whether the inflammation on my vocal cords and in my nose is wegeners granulomatosis or ‘unusual’ presentation of RA. The CA joints apparently look fine but there is lots of inflammation and subglottic stenosis. I read the article to which you linked and it seems that all of these symptoms could well be RA and not yet another hideous autoimmune inflammatory condition. I believe they use different meds for wegeners so it will be important to determine whether or not I have it. Thus far the prednisone eave put me on has helped somewhat.
Lisa, I’m so sorry you’re dealing with so many medical complications. I can’t answer your question because there are so many specific medical indicators for each disease. If it were me, and I were in your shoes, I would read every bit of information I could on Wegener’s and I would read what I could about the manifestations of RA in the throat (and other parts of the body, too).
I’d even make a 3 column checklist of symptoms that I had that fit one disease (column 1) or the other disease (column 2) or both diseases (column 3). I’d share this with your doctors. I’d also ensure I had an excellent system for keeping copies of medical records.
I’m encouraged to hear you are being seen by a team of specialists. Try not to get discouraged or overwhelmed as all the different puzzle pieces should eventually combine to make a complete picture.
I don’t know all the specialists who are on your team but some that come to mind would be: Rheumatologist, ENT, Neurologist, Respirologist, Immunologist, PCP, Endocronologist. I would want to ensure that I was getting the best medical care possible from the best specialists possible. Do you trust your PCP and Rheumatologist? Those two are probably very key for you. I would investigate who or where in the world the specialists are who manage patients with Wegener’s and RA. During my first year of RA, I spoke with or corresponded by email with some of the leading rheumatologists. Some were at the Mayo Clinic, some at Leeds in the UK, in Seattle, etc… It never hurts to email or be in contact with specific questions or to request information.
I wish you well. I hope you have good resources to help you cope with the emotional and spiritual toll this most likely is taking on you. I’ll be thinking about you and praying, too.
I had a bout of this a few years before my RA symptoms. Dr said it was psychological….ummmm….no! I bet it was an early flare…
This is interesting. I had an episode of feeling like something was in my throat and trouble swallowing over a year ago. It drove me crazy but seemed to subside after several days. Recently, just before my official diagnosis, I had a mild sore throat that quickly turned to laryngitis that lasted a good week or so. Perhaps it was connected to the RD after all!
YES! This is me too! For several months now, my voice comes and goes and has NOT been normal during this time. I also have a cough no one seems able to diagnose. I have an appointment with an ENT doc tomorrow – will be curious what he has to say. I am taking the email with me about this. I also have developed a screeching in my ears during these past months from about when my voice went whacko. I’ve wondered if it’s my RD!
Well…the ENT doc put a mirror down my nose into my throat and claimed he “sees something” on my vocal chords and needs to do a biopsy on it…makes me even more confused! It has yet to be scheduled at the hospital. I have no sore throat like some of the others who have commented. I still suspect my RA and wonder if this biopsy is really necessary. I have a follow-up 13 Feb with my rheumatologist so I am going to run it by him.
The same thing happened to me – something on my vocal chords. Had a biopsy done – general anaesthetic – had extreme difficulty intubating me – chipped teeth, lacerated tongue and haematoma. Discharged – back next day in intensive care with airways threatening to collapse. Have all the symptoms of cricoarytenoid arthritis – never picked up.
I have a fairly wonderful Rheumy, but still can’t get her to acknowledge that my loss of singing ability is anything but age.
I can’t sing and can’t read aloud to my kids, I can’t talk on the phone more than a few minutes.
My sweet hubby notices when I am going downhill, and says “yeah, your voice is getting “wispy” so I know you’re flaring.” Why don’t the doctors see it?
Sounds like me. Croaky voice usually when we are about to get rain.
Sometimes find it hard to swallow my tabs.
Sore throat Yeah that’s me alright.
Rheumatologists have just said never heard of it before
Not too long after I had been diagnosed with the disease I was talking on the phone with my best friend from high school. I hadn’t spoken with him in over 15 years and he commented to me several times that my voice sounded different. I attributed the difference to the fact that I had stopped smoking. But now…
Interesting article…..My ear, nose and throat doctor found mine. He found the affected joints and asks me if I had RA and I said, not that I know of….then he referred me to Rheumatologist and low and behold there it was.
thanks for sharing Pam. We’ve seen as the “first” symptom almost any “joint” / moving part.
This article is timely. My friend with Lupus has been waking up with a hoarse creaky voice, and was wondering if it was related to her inflammation / autoimmune disease. Just sent her this article, she was starting to feel crazy wondering why.
I get a lump-like feeling in my throat, like a swallowed a huge bite of mashed potatoes and it stalled halfway down. It aches slightly when I swallow. It mostly comes on when I’m flaring badly, and not that frequently in my life. I didn’t realize it was related, I always assumed that somehow it was related to swollen glands (which only happen to me in my underarms during a flare, never the neck), or fighting off a cold that never happened. I’ve had my thyroid checked endlessly too. This is so interesting. Thank you Kelly for posting about these related issues!
This issue of RD in the vocal chords or in the throat is very interesting. After reading other articles by Kelly on her experiences I told a friend her voice was not “smoker’s voice” from less than a year of smoking in her youth. I also told her I did not believe some of the extreme hoarseness that came and went was related to allergies. Given other on again off again health issues I really thought she might have RD. She is now functioning better. Not her full self but much better with treatment for her RD.
Like Sally I went to an Otolaryngologist (wish they still were ENTs) and then on to a gastroentroalogist. My issue was not loss of voice, it was the reoccurring gagging, swallowing and upchuck.
Neither the Rheumy or the other two specialists would put the new issues together with this so fun rheumatoid disease. But atleast I was not treated dismissively.
Turns out there was quite a bit of inflammation, even ulcers in the esophagus caused by; yes that’s right; medications for the RD. A change in the NSAID and addition of another medication to protect the esophagus, etc…
Be very cautious with Ibuprofen and its relatives at high doses and daily use.
`Question: how to get specialists to talk or even read with open mind each others conclusions on you/me the patient??
NVk
In addition to the CA and other issues mentioned by Kelly and all above, Thyroid disease can also carry many of these symptoms (the lump in the throat, hoarseness) and is a very common co-morbidity with RD. Typically, they are both autoimmune (Hashimoto’s Thyroiditis), but not always. Anyway, another throat involvement that should be investigated along with all the others – and another reason why a non-dismissive doctor and excellent diagnostician is important (and, oh so rare, it seems!).
I was hospitalized for this about a month ago but it was never diagnosed. They treated me for an infection. I had the sore throat, felt like something was stuck, lost my voice for about 4 weeks. They put me on antbiotics and lage dose of prednisone and it got better. I have great rheumtologist, he wasn’t there when I was hospitalized, and since I had gotten choked they assumed it was infected then my lungs got involed. I go to my regular RA DR. next Monday can’t wait to bring this up with him. My voice goes away all the time and has for months but I never brough it up to him because I never dreamed it was related! Thnkyou so much I have learned so much bout RA from this website. I have Feltys syndrome and Sjorgren’s disease and Im trying to manage it all plus be a 24/7 caregiver to my mom who suffers from Alzheimers disease. I get overhelmed alot I figure one of these days dealing with both diseases I will just ‘foget’ I have RA! Sorry bad joke. My motto is Appreciate the good, laugh at the crazy and deal with the rest!
I saw an ENT for an unrelated issue (clumsy me fell and broke my nose two weeks ago). I took the opportunity to ask him about my voice. I studied voice in college and have sung in choirs and community theater consistently since then. About 8 years ago I started losing my upper range. I have gone from a 3+ octave (I used to hit the E above high C) singing range to half of that and can barely hit a C on the staff for those of you who know music. The ENT responded, “The Larynx is a joint and between RA and GERD from the medications for 25 years, it’s pretty common.” He told me he’s done multiple clinicals with Rheumy’s and has seen it in his practice.
Thanks for sharing the story Laura. Sounds like you found a good ENT doc. I’m sorry it’s taken such a measurable toll on your voice.
Pingback: MEDICATIONS AND MAHI MAHI WHO KNEW? - The Diary of an Alzheimer's Caregiver
Does anyone know if the inflammation of the cricoarytenoid joint is also a symptom of Rheumatic Fever? I have just recently developed pain in my throat (not a sore throat, but the feeling of fullness, like something is stuck, labored breathing, loss of voice or other than natural ranges, etc.), in addition to pericarditis and pleurisy. I have NO joint pain anywhere in my body (other than my throat, which I just realized is a joint). One Dr. says I have RA, but another says no way without joint pain. The other Dr. thinks I have RF, but am waiting for a strep culture. NOT ONE DR. WILL ACKNOWLEDGE MY THROAT PAIN, WHICH HAS ALWAYS BEEN THE START OF EVERY FLARE UP AND OFTEN MY CHIEF COMPLAINT. They ALL say it is referred pain that is just an extension of the inflammation from my pericarditis/pleurisy, which is just around the lungs and heart. Any thoughts/ideas??
well that explains why sometimes it feels like i got punched in the neck and it hurts to talk. THanks for the info!
Interesting. I have RA and have had it in my hands for 30 years-never any pain. I now finally have a firm diagnosis of RA. I have been treated for spasmotic dysphonia ( vocal cords go into spasm and it is hard for me to get people to understand what I am saying). I go to a specialist for botox injections in my vocal cords twice per year to stop the spasms. I wonder if this is related to my RA and no one connected the dots.
thank you for publishing this i lost my voice for 6 month right before the the RA came on hard the Rheumatologist and ENT said it was gastro-esophageal reflux disease (GERD)kept ordering test and scans and never showed anything i told them there was something else going on they ignored me kept giving ant-acids then dx’d with RA and still said it was reflux.
THis explains why i lose my voice every year not from a c old which i don’t get but the feeling of a bone stuck down in my throat that i can’t get out then the loss of voice.
it is really depressing that i had such a great singing voice and lost it and when i said it that to the ENT he said well if you don’t do it professionally then no big deal ..what and a%%
Hi Kelly this is off topic but I havnt seen you on FB in a long time. Did you quit using it? Havnt heard a word from you since May I guess. What’s going on? Thanks Judi Barry
Hi Kelly, Thank you for copying these links to me abou thte larynx “JOINT”. Im not the patient,I’m the spouse of a RA patient. Its been 4 years since being diagnosed and I think this is the worst year yet. Amongst a SCHLOOOO of side effects and add on conditions, at the end of September, my husband lost his voice or it went really hoarse. It was a few days after his last epidural pain injection in the back of his neck. They ruled out any relation, however, I am still tilting my head wondering about it. He was having breathing issues, but he also has had asthma since he was little. We thought his asthma went from needing a pump every once in a while to needing a nebulizer treatment 3 times a day. We’ve seen the Pulmonary doctor, had a sleep study, pulmo function test, upper GO barium CT scan, seen an ENT, he did one scope visual a month ago, little redness, swelling & strain vocal cord, he doubled acid reflux meds, just went for a recheck yesterday, he did another scope visual, no improvement, same redness,inflammation and strained vocal cord, his advice: over a certain amoutn of time, you tend to develope bad habits such as “MAKING” your voice sound like that, so since the acid reflux dosage change didnt help, lets try speech therapy to teach you how to speak correctly. I was soooooooo flabber ghasted. I wanted to scream. I asked if it could be RA related, he said yes. I asked if the inflammed larynx could cause breathing issues, he said, well, it isnt opening up correctly, but no. (??????) I was so angry!! The RD said this has no RA relation because all the blood levels are clear. I did contact the primary and she is referring us to UCSF. The only thing that came back was a small hernia in the throat lining. (????)I’ve read a lot of the cricoarytenoid cases and he has allthe symptoms, I’m scared that UCSF wont accept the case because all the blood work is normal and all test were normal. They are asking me for the records and they are all clear. This is WAY beyond a MILD case of asthma. A person doesnt go to needing a nebulizer once in a while to needing one 2-3 times daily or lose their voice for months on end….. Do you have any suggestions. We have an appointment with the RD on Monday and I dont even want to see her, Im so irritated…. All I want is some healing and my husband to have some sort of quality of life back! He’s 46 for Pete’s sake. :/ Mean while, he still is very very hoarse and extremely tired from having issues breathing, he’s in pain. He had to stop the Humaira because they treated him for peumonia – Humaira does not take away much of his pain but it help the blood word to read clear…………
Helpless in Tracy,
Desi
Sorry for all the spelling errors. I was trying to type fast. Im at work. :/
Wow –I have to believe The Lord allowed me to see this today–there are no accidents in life! I now know what all of “these things” are and have been for all this time. I will bring this all to my rheumy at my next appointment. I have or have had every single symptom on the list. I recall they first showed up either during or before a severe flare. I have suffered with RA for 25 years and also now have Sjogren’s and Fibro. The Sjogren’s has given me a lot of nose, eye, ear and throat issues. The ears seem to have been a bigger issue since the throat problems started. Thank you so much for all the info–I will continue to research and educate myself.
I have been diagnosed with both Lupus and RA and over the past year, I have started having a “lump” in my throat. I am a police dispatcher and I have trouble getting sound out sometimes during a “flare”. I just fired my Rheum when she said that my 2 positive ANAs were just flukes and my symptoms needed to be managed by my PCP. When I questioned her, all my meds were cut off. She refused to fill my Simponi, Arava, and other meds so right now, I am flying without meds. Some doctors just don’t get it. I have an appointment with a new Rheum, so maybe this one will have some brains. Thanks to this article, I will be better able to tell him about this problem and actually have a name for it.
Thanks for posting this! I went to the doctor yesterday for what I thought was something stuck in my throat. He took one look, stood back, and said, “Does arthritis run in your family by any chance?” I told him about my RA and he was like, “Bingo!” I had no idea that this could even be a symptom of RA, but it is comforting to know that there are doctors out there who are informed. Your site is always the perfect place for finding information on these sorts of things, I really appreciate it.
I have started to notice my throat bothering me and it comes and goes. It would hurt to swallow and then when that went away it would feel like I have phlegm in my throat that I couldn’t get rid of. I always thought that maybe I was coming down with something but I would never get sick or that it is the remnants of when I was sick 2 months ago. With everything out there I just don’t know what to think anymore and how long have I really dismissed so many ailments before I was diagnosed.
So, I’ve had issues with feeling epiglotis is swollen…it gives me panic attacks. Is there any options besides regular RA meds?
This is very interesting. I have had a violent cough multiple times a day that starts with a tickle in my left throat. I have had more sore throats and difficulty swallowing since diagnosis of RA 1 year ago. I am constantly clearing my throat and become hoarse. I have discussed with both my Rheumatologist and my GP and neither are too concerned and blame the cough on my BP med (which used to give me similar cough but had gone away years ago). I will request a consult with ENT. I respect my Rheumatologist – but I think some of these “rare” issues are more common than the research and literature have recorded.
Love this site! Have consulted and read a lot but never posted before.
This site is awesome!
I’ve lived with RA for 34 years!
During the past three and a half weeks I’ve been experiencing some symptoms which are similar to those of CA which can be caused by RA.
Very informative site. Thank you Kelly!
From time to time i will get a feeling of a lump in my throat , it only lasts for a few days , but never found out what it was, learn something every day.
I have been reading and reading about RA for a couple of months now. I am extremely sad. I cannot think of one part of my body that hasn’t been attacked. Laryngitis several times and now loss of my singing voice–the upper range. I love to sing. I also have ELP in my mouth and my girl parts. Very painful. It has taken my smile (hurts) and my sex life. Singing smiling and sex. Just about wraps up my life. My feet were the first to go. I have huge gnarly bones sticking out like bunions. They started to form about 30 years ago. Silly me I thought it was because I wore cheap shoes! Now I can only wear shoes with roomy toe beds. No pumps or high heels—- not that I ever wore them.
Low thyroid.
Very high cholesterol.
Tinnitus
Roving back pain (my term)
Hot swollen burning thumb joints
Dry eyes
Hair loss
Alopecia
Vitiligo
Tired
And on……
Have a Rheum dr appt in March.
Well this is been enlightening for sure!! For the past 5 years I’ve been trying to figure out what’s going on with my throat! I have been to countless doctors because I have a lot of mucus stuck in my throat is extremely sticky and very very difficult to cough or spit out so much so I believe I bruised my ribs trying to cough and spit it out because of the pain I develop it is a violent ordeal. I am now on a nebulizer that makes it easier to cough up and spit out but it’s still constant. I also take lots of Mucinex and feel the need almost constantly it gets worse when I eat. My pulmonologist thinks it’s the Sjogren’s and that’s the only answer I’ve gotten for 5 years. When I wake in the morning it’s almost impossible to get my voice to work and have anyone understand me it is so low and difficult to talk. Has anyone else experienced this horrific mucus that is truly ruining my life!! I hope and pray someone has some answers and I can get better finally!! I have a multitude of autoimmune disorders some doctors differ whether I have Crohn’s or UC. I have been diagnosed with achalasia and Barrett’s and another doctor tells me I have hypertensive Les instead IDK I am so tired of going to doctors and getting nowhere 🙁 I believe I got my diagnosis of RA in 2006 and have been on Humira ever since. I did go off of it for a little while to see if that was causing the problem and nothing changed except I did feel more pain than normal. I finally got a doctor to test the sputum and it came back staff and they treated me for that but it’s still pretty much feels the same.. sometimes I spit out and cough up very dense material that is extremely sticky always whatever consistency and sometimes it’s clear and sometimes colored but ALWAYS there. When they have x-rayed my lungs they say they’re clear. I also have Gerd/ reflux now my brain fog is kicking in!! I have been to the ER before after using the Neti Pot n I felt like I was drowning it was stuck somehow IDK?? But they did nothing for me at the ER so I quit going. I choke easily I can feel the yuk in my throat and I believe that’s what makes me choke sometimes when I’m eating… the influx of the “yuck” If anyone has any idea of what I could do to help this I would appreciate it and no I don’t drink milk I’m lactose intolerant. I’ve tried everything over the past five years pretty much but I’m sure there’s an answer out there I just have not found the right doctor or talk to the right person.I was diagnosed with Graves disease as well many years ago. I’ve seen several ents several gi’s and have stayed with the same rheumatologist he’s at least nice…
I don’t know how informed he is but he listens and I feel like he tries . Thank you for all this valuable information and please if you can help me I would be ever so grateful!!!
Hi Bee,
CA is very common in RD, affecting as many as 90% of patients according to research I read for my book on RD. Your symptoms could be from that, or may be caused by one of your other diagnoses.
Oh my goodness! I have (and have had) 10 of those symptoms! I sing semi-professionally, and have been battling this stuff for especially the past year, but some of the symptoms showed up in my early 30’s! (I’m 65 now, and just a year ago began seeing a rheumatologist.) About 4 years ago I was singing everyday anywhere from 2 to 6 hours straight! And had no problem, not even hoarseness after so many hours of singing. I was at the peek of my vocal capabilities and in demand for weddings and funerals locally. I sang a lot in church, solos and choir, and had a range to be able to sing many octaves. Then the hoarseness began, followed by the dry cough, and now, most prominent is the feeling like a toothpick is poking at the back of my throat, whenever I attempt to sing. Plus the jaws painfully lock up and create a charlie horse, after a mere few minutes. I am really surprised that this is actually a part of it all!! Thank you for this discovery! I was about to begin searching for a doctor who specializes in voice components.
Desi – Helpless in Tracy….
I’m wondering if you have Kaiser. If you do, I can give you the name of the Chief Rheumy in Walnut Creek – Kaiser. She’s accepting new patients right now and she is more thorough than ANY past Rheumy I’ve had.
Let me know if you have interest.
I hope this finds your husband doing better. I got the run-around with TWO Rheumys until I found this one. I hope to NEVER change.
-Tiffany
No one has posted on here since April 2018 but I’m going to post anyway. I was diagnosed with RA in 2006. In 2014 I started noticing changes in my voice when talking. I have a lot of sinus issues and drainage and chalked it up to that. The vocal issues would come and go. I started noticing it more in 2015. By that time I was taking care of my elderly mother who was in failing health. My friends would ask what was wrong with my voice, but I was so caught up in caring for my mom, I just dealt with it on my own. Finally, in 2016 I went to an ENT. He did a laryngoscopy by putting a tube with a tiny camera up through my nose and down into my throat. He viewed everything the camera showed on a screen in front of him. I had previously read up on RA and how it can affect the voice. I went over that with the nurse in my medical history and pointed out what I had read about RA/vocal issues. I also talked to the ENT about it before the test. He didn’t respond to what I said at all. As he was running the test he mentioned I had a bone spur inside my nose and then made fun of me by saying to the nurse, “We got a mouth breather here.” I presume that was in response to all my sinus issues. Once the test was completed, he said he found no signs of cancer, no polyps, no nothing. I had also mentioned to him that I get dry mouth from time to time but only when I wake up from sleeping and sometimes have a horrible taste in my mouth along with the dry mouth. He said that was caused by acid reflux. Before the test, I mentioned that I have issues with anxiety and OCD. And, that I notice my voice is always worse when I get nervous. or worrying. After he announced he found nothing wrong with my throat, I asked him then what was causing my vocal issues, he looked at me and said, “You are.” I had no idea what he meant, so I asked how I could be causing my hoarseness. He said it was me because of my anxiousness. I had never heard of such a thing. I told him I had thought it was RA related he said no it’s stress and anxiety. Then he said he was sending me to see a speech therapist for further diagnosis. I went to the speech therapist, who turned out to be a third cousin of mine. She was really understanding and said she had the same issue once, and found out she had Celiac Disease and stress combined to cause her vocal loss. She had me do some vocal exercises and determined I had either muscle tension dysphonia or spasmodic dysphonia. After a few more vocal exercises, including putting my head down almost between my knees while saying a series of exercises, she determined I have muscle tension dysphonia. I again mentioned having RA and I even gave her some printouts I had made from websites on the subject of RA and vocal issues. She read them over and said that if that were the case she couldn’t help me with my vocal issues, however, she believed that due to my high level of stress and anxiety it was not RA related but muscle tension dysphonia which is believed to be brought on by stress. At that particular time, my stress level was huge as my mom was seriously ill and in and out of hospitals. And I was her only caretaker. Knowing my stress level was huge at the time, I went along with the diagnosis of muscle tension dysphonia. My speech therapist said if I had spasmodic dysphonia it could be treated with botox shots, however, the form I have, muscle tension, the only treatment is speech therapy. She said I needed to learn to change the way I speak and raise the tone of my voice. She gave me several sheets of vocal exercises to work on and had me come back for another session. I have done a lot of theatre in the past so I was used to doing these types of vocal exercises for warm-ups. She wanted me to come back for some more sessions but unfortunately, my insurance was lousy. I had to pay for the initial diagnosis session out of pocket which was $300, and the further half-hour sessions were $250 and my insurance only paid $20 of that. So, I couldn’t afford to go back. Since my speech therapist was also my cousin she gave me extra exercises to work on and some more info to read. She told me I was a mess from stress and suggested getting some cognitive therapy and try yoga and meditation. After that, I worked on the vocal exercises but find that they irritate my throat. I sometimes have days when it’s fine and others it’s horrible. Everyone keeps telling me it’s stress. My mom passed in late 2016, and I had to deal with all that, still am actually. Losing my mom was horrendous. I was also in charge of her estate which was a nightmare to deal with and just finally got that settled in the spring of 2018. The past 3 months I went to see a psychologist for cognitive therapy. She blamed everything on my anxiety and gave me a prescription. But, nothing has helped my voice. I was not working during the time of my mom’s illness because I was her full-time caretaker. Now I need to find a job and my voice has gotten bad again, and I’m afraid to apply for jobs and have to deal with job interviews with my voice the way it is. When my voice gets bad I hate going any place I have to be waited on, like a store or restaurant because people hear me and think I have a cold or something contagious. I find myself apologizing all the time for the way I sound. And, I find the stress of going anywhere makes my voice worse. I’m just getting really tired of dealing with it and feel like some sort of freak because everyone I talk to has never heard of such a thing. Last year my former dentist recommended I go an ENT in a neighboring large city. He said he highly recommended him. I recently looked him up online to call about an appointment and I read he and his wife are being sued. She was practicing medicine without a license and he was knowingly letting her use his office to do it. He has since moved out of state. I thought great I finally try to get in with a good ENT and find out he’s done something illegal. I feel very isolated dealing with my vocal issues so having found this forum has really helped me to feel I am not alone. I wish everyone the best .
I am so incredibly glad that I found this site, and this particular post, even though it was originally posted so long ago. About 3 months ago I was diagnosed with inflammatory arthritis (but not RA, definitively).
Aside from the crushing fatigue and joint aches, since January I have had:
– sore throat (on the left side)
– hoarseness
– a lump-like sensation in my throat
– left side chest pain
– slight cough
So far I have seen an allergist, an ENT, a gastrointestinal doctor, a cardiologist and of course my general practitioner. I have had a chest x-ray, a nuclear stress test, a chest ct scan, a barium x-ray and I have an endoscopy next week. So far everything is normal and my doctors are pretty much ignoring my sore throat. My GP wanted to give me anti-anxiety medication, which I refused, because I am a pretty non-anxious type. Thank you so much for posting this, and for all of the replies, I finally feel like I am not imagining all of this. I am going to schedule another visit with my rheumatologist and follow up with him. Thank you, thank you, thank you.
I HAVE 2 CASES WITH HOARSENESS OF VOICE AND ODYNOPHAGIA ONE RA AND ANOTHER ONE IS NOT RA JUST C\P OF HOARSENESS OF VOICE , I TREATED THEN BY PERINEURAL INJECTION THERAPY 4 SESSIONS WITH COMPLETE RESOLUTION OF SYMPTOMS EITHER CLINICALLY OR BY INDIRECT LARYNGOSCOPE